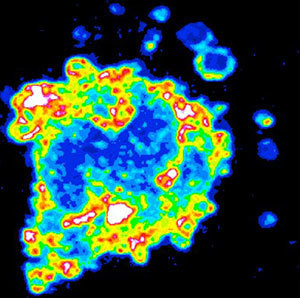
 Tumor cell surrounded by shed microvesicles
Tumor cell surrounded by shed microvesicles
Over the past few years, extracellular vesicles, or membrane sacs secreted from cells, have emerged as important mediators by which cells communicate with their surroundings to regulate a diverse range of biological processes. In addition, specialized roles for extracellular vesicles are beginning to be recognized in various diseases including cancer, infectious diseases and neurodegenerative disorders. Moreover, engineered extracellular vesicles are likely to have applications in drug delivery.
The laboratory of Crislyn D’Souza-Schorey, Morris Pollard Professor and Chair of the Department of Biological Sciences at the University of Notre Dame, has been investigating a unique population of vesicles released from tumor cells.
“We refer to these vesicles as tumor-derived microvesicles,” she said. “Our work over the past few years has focused on their role in enhancing tumor cell invasion. Emerging evidence suggests that extracellular vesicles can propagate cancers in several ways — for example, by breaking down the extracellular matrix to allow tumor cells to invade their surroundings, by enhancing angiogenesis and by possibly modulating the patient’s immune system, all of which promote metastases.”
In cancers, the number of tumor-derived microvesicles in circulation increases with disease stage. Not only are they provocative targets for therapeutic intervention, they are also potentially rich reservoirs of clinical biomarkers, D’Souza-Schorey noted. Despite this, there is only a rudimentary understanding of how this specialized subset of membrane vesicles is shed from tumor cells.
“We know that it is not random release from cells, but that tumor cell components are targeted to these vesicles before they are pinched and realized from cells,” she said.
In a study published Tuesday (April 21) in Nature Communications, her research group provides insight into how certain proteins may be directed to tumor microvesicles. They show that a protein called VAMP3 guides key components of the cell toward shedding microvesicles to help facilitate extracellular matrix breakdown and tumor invasion.
“Getting at this type of information is important because it provides options for how one might be able to modulate the composition of these shed vesicles or prevent release,” James Clancy, the lead author on the study, said.
The study also shows that microvesicles were identified in the blood and ascites of women with ovarian cancer.
“We think that these microvesicles are shed into circulation universally by tumors, and began testing this hypothesis by assessing the body fluids of patients with ovarian cancer,” D’Souza-Schorey said.
This was aided in part by collaboration with physician oncologist Michael Method and his team at Michiana Hematology Oncology. The collaboration was initiated several years ago, when the laboratory first identified these microvesicles in their tumor cell cultures.
“We sought to investigate whether this population of microvesicles could also be detected in the body fluids on cancer patients,” D’Souza-Schorey said. “Dr. Method not only provided oversight of the clinical samples we obtained, but he also walked us through the pathophysiology of the cases we were investigating.”
The study shows that CA-125, a commonly used serum biomarker for ovarian cancer, is highly enriched in microvesicles isolated from ovarian patients. These findings suggest that the development of microvesicle-based biomarkers has the potential to enrich key tumor markers and enhance the sensitivity of detection. These results are particularly timely as there is growing interest in harnessing circulating microvesicles as disease biomarkers.
The study was supported in part by a grant from the National Cancer Institute and the Advanced Diagnostics and Therapeutics Strategic Research Initiative at the University of Notre Dame.
Contact: Crislyn D’Souza-Schorey, 574-631-3735, Crislyn.D’Souza-Schorey.1@nd.edu